PatientQuestionnaire-v2.1(EN)
Inhoud
[verbergen]General information
Name: nl.zorg.template.PatientQuestionnaire ![]()
Version: 2.1
HCIM Status:Final
Release status: Published
Release date: 5-7-2024
Metadata
| DCM::CoderList | * |
| DCM::ContactInformation.Address | * |
| DCM::ContactInformation.Name | * |
| DCM::ContactInformation.Telecom | * |
| DCM::ContentAuthorList | * |
| DCM::CreationDate | 15-05-2020 |
| DCM::DeprecatedDate | |
| DCM::DescriptionLanguage | nl |
| DCM::EndorsingAuthority.Address | |
| DCM::EndorsingAuthority.Name | * |
| DCM::EndorsingAuthority.Telecom | |
| DCM::Id | 2.16.840.1.113883.2.4.3.11.60.40.3.21.2 |
| DCM::KeywordList | |
| DCM::LifecycleStatus | Draft |
| DCM::ModelerList | * |
| DCM::Name | nl.zorg.template.PatientVragenlijst |
| DCM::PublicationDate | |
| DCM::PublicationStatus | Unpublished |
| DCM::ReviewerList | |
| DCM::RevisionDate | 05-07-2024 |
| DCM::Supersedes | nl.zorg.template.PatientVragenlijst-v2.0 |
| DCM::Version | 2.1 |
| HCIM::PublicationLanguage | EN |
Revision History
Concept
A patient questionnaire is a structured questionnaire in which a care professional asks the patient or a contact person a number of questions about his health, (disease) history or experiences during a care process.
This is a template HCIM. For actual use, meaningful element names and filling of the value lists will have to be provided for derived HCIMs.
Purpose
The purpose of a patient questionnaire is to request information from the patient that is important to know for the treatment, the result of a treatment or his experiences in the care process.
Evidence Base
When using standardised questionnaires, it is common, especially when repeatedly completed by the same patient or client, to vary the order in which the questions are presented. The aim of this is to avoid automaticity in filling in the questions.
As response options for the questions in these questionnaires Likert scales are often used. These scales consist of a number of answer options to be defined per scale (5-point Likert scale, 9-point Likert scale,...). Here the filler indicates by means of a number between 0 and maximum, in these cases 0-4 or 0-8, to what extent the filler agrees or disagrees with the question or to what extent the statement applies. For the same reason the order of the questions are rotated, the mapping of the answer options to the numbers are sometimes reversed. As an example, choices from 'Very bad' to 'Very good' are then mapped to 7-0 instead of 0-7.
The template (and when applied in derived HCIMs) assumes that the application logic ensures that the information from the completed questionnaires is processed in such a way that these differences are not reflected in the information represented by the template or derived HCIM’s.
Although other arrangements can be made when using a derived HCIM, it seems logical to opt for the option of always choosing the mapping 'negative -positive' to 0 - maximum for recording in accordance with such a HCIM. This unless the original instrument has very specific instructions for this.
The order of the questions in the questionnaire presented to the patient is not reflected in the template/derived HCIM as the questions are identified by the name of the element that represents this question and the concept ID associated with this element.
Should in defining derived HCIM the choice is made to use element names such as 'Question 1', the number in the question never refers to the place in the presented form, but at most to the place in the questionnaire definition. To avoid confusion, it is better not to use this kind of names.
If the template and derived HCIMs are applied in accordance with the above, the information from their instantiations can always be compared without editing, preventing misinterpretation.
In the template or derived HCIM‘s, this concept-id will be used as identifier of the original question, the concept as data element and the linked answer to the question. If necessary a mapping table can be used for the original questions from the instrument, to the concept representation as data element in the derived HCIM and the fitting answer.
Information Model
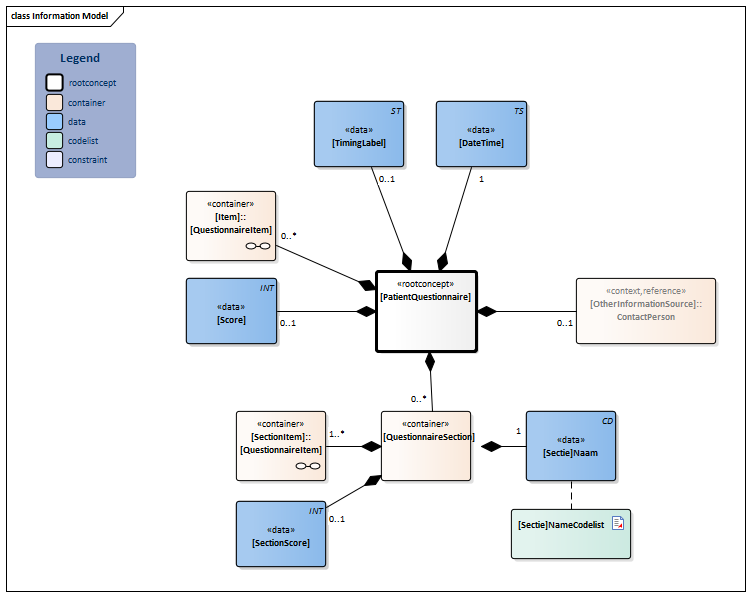
| Type | Id | Concept | Card. | Definition | DefinitionCode | Reference | |||||||
| NL-CM:21.2.1 | Root concept of the [PatientQuestionnaire] template.This root concept contains all data elements of the [PatientQuestionnaire] template. | ||||||||||||
| NL-CM:21.2.45 | 0..1 | The (total)score calculated on the basis of the answers to the questionnaire. | |||||||||||
| NL-CM:21.2.24 | 0..1 | The relative moment in time when the quesionnaire is completed (e.g. at 12 years old, before surgery, 5 years after implantation) | |||||||||||
| NL-CM:21.2.38 | 1 | The date and time of completing the questionnaire. | |||||||||||
| NL-CM:21.2.36 | 0..1 | If the questionnaire is not answered by the patient, the person involved in the care for the patient (parent, caregiver, ...) who answered questions about the patient. |
| ||||||||||
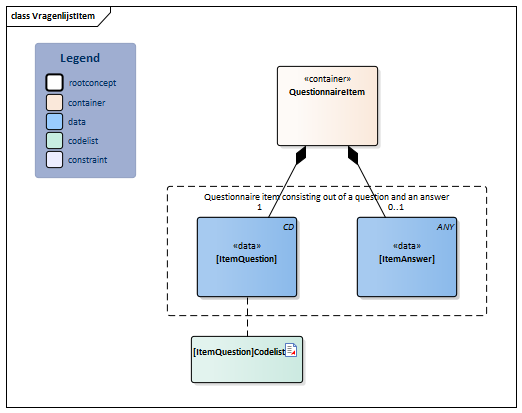
| NL-CM:21.2.43 | 1..* | Container of the [SectionItem]::[QuestionnaireItem] concept.This container contains all data elements of the [SectionItem]::[QuestionnaireItem] concept. | |||||||||||
| NL-CM:21.2.12 | 0..* | Container of the [QuestionnaireSection] concept.This container contains all data elements of the [QuestionnaireSection] concept. | |||||||||||
| NL-CM:21.2.27 | 1 | The name of the section of the questionnaire. This usually relates to the specific subject of the section in the questionnaire. |
| ||||||||||
| NL-CM:21.2.18 | 0..1 | The total score of the section calculated on the basis of the answers to the section part of the questionnaire. | |||||||||||
| NL-CM:21.2.28 | 0..* | Container of the [Item]::[Questionnaire] concept.This container contains all data elements of the [Item] concept. | |||||||||||
Columns Concept and DefinitionCode: hover over the values for more information
For explanation of the symbols, please see the legend page ![]()
Instructions
With this template, single HCIMs can be made that model one questionnaire with one or more sections.
If a HCIM of a questionnaire becomes very large and it contains a complex flow with conditionally visible or hidden questions, the modeller may decide to divide it into several smaller HCIMs. Alternative is to model these (pre-)conditions in a HCIM with the help of constraints.
It is also possible to refer to a website or place where this information can be found instead of doing this in a HCIM.
The sequence of completing and exact design of a questionnaire may be difficult to described in a HCIM and this is actually not what an HCIM is intended for. This information must be available from the publisher or creator of the questionnaire. not a modeller of an HCIM. The publisher is also the content manager of a questionnaire.
With every change by the content manager, one should check and track whether a single HCIM must be adapted.
The version management of validated questionnaires in particular requires attention and can be complex due to various translations in circulation.
Valuesets
[ItemQuestion]Codelist
| Valueset OID: 2.16.840.1.113883.2.4.3.11.60.40.2.21.2.7 | Binding: Example |
| Conceptname | Conceptcode | Codesystem name | Codesystem OID | Description |
[Sectie]NameCodelist
| Valueset OID: 2.16.840.1.113883.2.4.3.11.60.40.2.21.2.4 | Binding: Example |
| Conceptname | Conceptcode | Codesystem name | Codesystem OID | Description |
Previous versions of this template
- PatientQuestionnaire-v2.0 (01-09-2022)
- PatientQuestionnaire-v1.0 (01-09-2020)
About this information
The information in this wikipage is based on Prerelease 2024-1
SNOMED CT and LOINC codes are based on:
- SNOMED Clinical Terms versie: 20240331 [R] (maart 2024-editie)
- LOINC version 2.77
Conditions for use are located on the mainpage ![]()
This page is generated on 05/07/2024 16:34:28 with ZibExtraction v. 9.4.8881.42943